| Trans | Internet-Zeitschrift für Kulturwissenschaften | 15. Nr. | April 2004 | |
|
2.7. Culture, Psychosocial Disorders
and Mental Health: an African Perspective Buch: Das Verbindende der Kulturen | Book: The Unifying Aspects of Cultures | Livre: Les points communs des cultures |
||||
Erhabor Sunday Idemudia (Ibadan/Nigeria)
[BIO]
Abstract
The various branches of the Social Sciences, including Psychology, understand that neither health nor ill health occur randomly within populations. Both are rooted in social processes such as the pattern of social interactions between individuals, groups or nations and people's reactions to and perceptions of their social, physical environments. There are also the overarching systems of values and norms, which help perpetuate patterns of mental health. According to Blue and Gains, (1992) cultures develop treatment models that reflect their own values. Unfortunately, most research literature originates in Western cultures producing an ethnocentric view of psychopathology that can limit our understanding of disorders in general and can also limit and restrict the way we approach treatment in Africa. The result is that African psychologists are being distracted and diverted from questions of the moment in their native communities. This has explained several omissions in the quest for African psychotherapy.
In this paper, the ways in which culture affects psychosocial health positively, negatively and recovery from the African perspective will be reviewed within the framework of the links between indigenous theories of conflicts/stress, solidarity and breakdown. Not only do cultural definitions influence the interpretation of an event as stressful, but also our understanding of the role of life events depends on the models of the mental health practitioner. For the mental health worker, the challenge is to detect the ways in which the interplay of social facts and relationships affects the patient's mental health. Therefore, it is important to every mental health worker to know, understand and be familiar with the cultural dynamics of the society he or she is working in. This paper intends to demonstrate how these cultural stresses express themselves in African patients. The paper will also attempt to bring some coherence to a series of observations made by people knowledgeable about the conditions of health and disease in Africa from a mind-body perspective.
Background
How can we begin to see mental health and psychotherapy through the eyes of culture particularly in African settings? Or put differently, what is the role of culture in psychosocial disorders, which help perpetuate patterns of mental health and recovery among Africans?
To see mental health and psychotherapy through the eyes of African culture, we must first know and understand clearly what mental health is all about and how it is conceptualised from the African perspective and afterwards, then begin to appreciate the most appropriate psychotherapeutic approaches to treating these problems.
The Kenya people will say "Shonyala okhumanya inzu yowasio tawe" which literally means that you cannot manage or know better the affairs of the house of your neighbour. According to Fridah Muyale-Manenji (1998), the parable is used when respecting one's privacy. Also, the saying is used when people assume they know what is going on in somebody's home.
I am writing this paper from the perspective that first I am an African and a clinical psychologist and have several years of clinical practice with African clients. It is my hope that this paper is well focused. If it is biased in any way, then that is because I have chosen to write from this perspective. To my mind, culture means the values and norms of people that make them live in a particular way. I see culture as a way of life of a people. In other words, the sum total of all things that refer to the religious roots of people: symbols, language, parables, idioms, songs, stories, celebrations and all expressions of way of life. It also encompasses kinship, ways of relating to each other, and even ways of expressing illness and yielding to treatment.
It is in the light of this background, therefore, that this paper will focus on the ways in which culture affects psychosocial health positively, negatively and recovery from the African perspective within the framework of the links between indigenous theories of conflicts/stress, solidarity and breakdown.
Introduction
The impact of culture and society on personality has been the subject of important investigations in psychology, but unfortunately the percentage of variance explained by culture and psychosocial disorders within the African community is something that deserves special attention. While trying to provide explanation for the relationship between culture and health, Harkness and Keefer (2000) observe that health and or illness are culturally defined and treated, since cultural meaning systems inform aspects of illness and some diseases are culturally specific. This observation implies that culture is a way of life of a people within the same given boundaries. How does this way of life within common boundaries reflect on mental health or psychosocial disorders or even on possibly recovery from psychological problems?
Unfortunately, most research literature originates in Western cultures, producing an ethnocentric view of psychopathology that can limit our understanding of disorders in general and can also limit and restrict the way we approach illness behaviour and treatment. The result is that African psychologists are being distracted and diverted from questions of the moment in their native communities. This has explained several omissions in the quest for African psychology.
The African Conception:
Africa is a continent that is culturally diversified. Although there are cross-cultural and ethnic differences in Africa, there is nonetheless a general belief that both physical and mental diseases originate from various external causes such as a "breach of a taboo or customs, disturbances in social relations, hostile ancestral spirits, spirit possession, demoniacal possession, evil machination and intrusion of objects, evil eye, sorcery, natural causes and affliction by God or gods.
According to Taussing (1980), the most important thing about society is the relationship between people, and as a result we need to recognize the human relationships embodied in symptoms, signs and therapy. Pearce (1989) also argued that "it is too simplistic to see disease as something physical, which attacks the body". According to him, disease causation can be due to "things we see and things we don't see". Many of the things we don't see are included in African belief systems, cultural and social values, philosophies, expressions, etc.
The African Attitude towards Illness behaviour:
How do the African attribute and perceives etiological factors of illness? According to Tsala Tsala (1997) every disease is systematically acknowledged as having a supernatural origin-the grief of ancestors or divinities, the practice of sorcery and various evil spells. To an African, biology alone does not explain disease causation, because it is seen as a social phenomenon, and as such has a significance for the whole ethnic group and immediate community members. Also Africans believe that diseases can be transmitted from one generation to another as long as the stains of a fault have not been cleared. Many collective rites exist, whose aim is to stop transmission of some diseases that run in the family.
The common element in the African belief system is simply that physical and mental illness is the result of distortions or disturbance in the harmony between an individual and the cosmos, which may mean his family, society, peers, ancestors, or a deity. According to Lambo (1978), for example, the African way of thinking does not draw a line between the living and non-living, natural and supernatural, material and immaterial, conscious and unconscious. These sets of phenomena, which in the west, are conceived of as opposites, are understood in Africa as unities. The seen and unseen exists in a dynamic interrelationship. Past, present and future harmoniously weave one into another. The dream world and the daylight world have equal reality.
In Africa, people interact with one another not on the basis of how things are, but how they perceive them. Africans perceive ill health to have material, moral, supernatural and pre-natural causes which can only be determined both by physical observation and divination (Ezeabasili, 1977).
According to Tsala Tsala, (1997) this way of viewing health and disease, as a matter of harmony or disharmony between an individual and a larger context is similar to the holistic perspective being advanced currently by Western researchers. (See Carlson & Shield, 1989).
Psychosocial disorders in the eyes of culture: (Theoretical Perspectives).
That culture influences the onset of psychosocial disorders and mental health is a theoretical as well as a practical reality.
Matsumoto (1996) defines culture as the "set of attitudes, values, beliefs, and behaviours shared by a group of people, but different for each individual, communicated from one generation to the next". From this definition he argued that culture is not rooted in biology, race and nationality. He also described the dualism in culture with the dimensions of individualism and collectivism (IC), which refers to the degree to which a culture encourages, fosters and facilitates the needs, wishes, desires, and values of an autonomous and unique self over those of a group. Detailed descriptions of both dimensions have also been written by Van der Walt (1997). According to Nefale and Van Dyk (2003), both dimensions are encountered amongst different groups in different parts of the world but in different degrees. The grading of communalistic and individualistic cultures may range from very weak and passive to very strong and active. In Africa for example, the communalistic culture has already started to change because of the dynamic nature of culture. These changes (stratification, integration, change, poverty, wars, famine, migrations) have brought about significant inner conflicts experienced by Africans.
According to Pearce (1989) these aspects of group life are seen as problematic, when, as a result of them, the individual finds a situation stressful. The concept of a stressor (noxious stimuli leading to sustained emotional arousal) has been well documented and viewed as the link between societal or institutional processes and the health of the individual (Innes, 1981).
Also, the links between conflict/stress and breakdown have also been recognised in indigenous theories of causation. Nzewi (1989) has documented the emphasis placed on good/moral behaviour and social harmony in the aetiology of health in among the Ibos of Nigeria. African societies (Yorubas, Ibos of Nigeria; Hehe of Tanzania, Luo in Kenya, the Amhara in Ethiopia) believe that disruptive behaviour and the breaking of taboos are punishable through misfortunes and ill-health.
Among the Ibos of Nigeria, Nzewi (1989) identified five ways of classifying psychosocial disorders: (1) Beneficial reciprocity - when an individual is unable to socialise adequately with his or her neighbours, since the "need to get along with everyone is a major concern in the interpersonal relationships among the people". (2) Degree of shame people experience (social conformity). According to the author, people who are well adjusted experience some degree of shame when he or she deviates from the norm of the society. Thus the Ibos of Nigeria consider as indicative of mental illness "behaviour which shows a complete absence of shame or scruples". (3) Non-directional/excessive, including disorientation to time. This is irregular/bizarre speech and motor behaviour (inappropriate behaviour). (4 ) Inappropriate affect and (5) Poor family relationship - when an individual is handicapped to the extent that his or her symptoms interfere with his or her fulfilling his or her family responsibilities.
Nzewi (1989) also went further to classify the different psychopathologies in the Ibo culture. Mentioned among the severe were: 'Onye nla' (mad person), 'Isi Mmebi' (diseased head), 'Isi Mgbaka' (sour head), Among the non-severe types were: 'Agwu' (possessed), 'Akaliogoli' and 'Efulefu' (indicating some personality disorders of different types, 'Ogbanje', etc. Please see Nzewi (1989) for details.
The African also believes that illness and health may depend on keeping in harmony with one's pre-life accord (Prince 1975). This is what many would refer to as "Destiny". Explained differently, when a person is born, he or she (due to an earlier agreement with God) lives the life that has been predetermined for him or her. As a result, deviations of any sort can then result in mental ill health. This concept also explains partly the belief in reincarnation (a continuous cycle between life and death). For example, the concept of "Ogban-Nje" (pathologic reincarnation) explains most forms of mental illness/possession, particularly among females in southern part of Nigeria. It is also a riverine phenomenon.
Also, some societies in Africa also believe that illness can even befall a relative for another person's wrongdoing. According to Pearce (1989), this idea appears to be similar to the Western view that defective interactions within a family could result in psychosocial disturbances in one member (the scapegoat). While the Western (social) perspective link outcomes to causes via naturalistic and mechanistic models (Freudian model based on physics), African social models use spiritual/religious idioms of explanation. Both models however, view illness as a sign of distress in social relationships in contrast to the traditional biomedical model.
|
Case histories:
|
The Body-Mind Psychopathology Link
According to Ebigbo (1989), a combination of cultural conflicts (conflicts, stratification, change, famine, externalised attitude toward illness) can bring about anxiety-related-types of psychopathology among Africans.
These psychic burdens emanating from such cultural conflicts need to be understood in the African perspective and idiom. According to Ebigbo, the body is the mind and the mind the body; therefore, physical images are often used to describe feelings of the mind and dispositions of the external mind (as in witchcraft), which are frequently attributed to the body. As a result, complaints of ill health, are always expressed physically, and the treatment is expected to be physical as well (Ebigbo and Ihezue 1982).
Psycho-physiological complaints are often formulated as subjective bodily sensations, including heat in the head and body, a sensation of worms crawling all over the body, a sensation of heaviness in the brain, the sense that the heart is melting and wants to fly away and a lump in the throat (Okhomina and Ebie (1973), Ebigbo and Ihezue 1982).
Several mental health researchers in Africa (Lambo 1963, Ayorinde 1977, and Ebigbo and Ihezue 1982) have described these complaints as the somatisation of emotional distress. These somatic complaints are usually presented by patients to obscure some psychic distress or, according to Morakinyo (1985), presented as "cloaked phobic states".
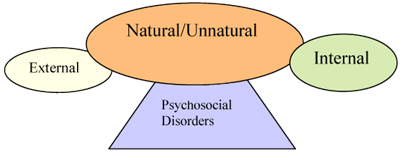
However, from my personal experiences with African clients, it is clear that physical and mental illnesses are seen and presented as a continuum, with one affecting the other. When Africans attribute causes to psychosocial disorders, this results from both natural and unnatural causes having sources of external and internal factors. This is illustrated in a diagram below:

Physical or Mental disorders can be attributed to
There is no doubt that the African prefers to use treatments that recognize their ways of thinking and their value system. A detailed description of different researchers on the nature of help-seeking behaviour and health-utilisation behaviour among Africans has been described (Idemudia 2003, Madu and Idemudia 1997, Idemudia 1995) and elsewhere (Gordon, 1990).
Given this perspective, how would what I would describe as a transitional African (transitional because they are more likely to seek the help of a psychotherapist) suffering from a mental problem be helped? A transitional African is one who has received Western education and as such has acquired both the African and Western values. The traditional African is firmly rooted in African values and has nothing to do with Western values. As Kleinman (1980) has pointed out, patients and healers have their own "explanatory models", that is, their particular understanding of what a human being is and how psychosocial disorders that may appear are to be accounted for and treated.
Let me illustrate further by quoting the work of Bourguignon (1989). This illustration shows that goes into deciding which treatment can be used. According to him, "there was a case in which a man suffered from impotence, with the result that his wife had not conceived, so their marriage was threatened". A diviner was consulted and "explained that the man's impotence was caused by the shade of his dead grandmother. In this case, impotence is then not seen as either a physical or an emotional problem, but one involving relationships with ancestors. According to him, the concern here is not so much with the man's dysfunction but rather with its reproductive or familial consequences. Here, the human being is viewed as one intimately integrated into a familial and social system and it is the social relationship with ancestors, spouses, and descendants that are investigated in cases of illnesses rather than physical or emotional disturbances.
It should be noted, however, that not only do cultural definitions influence the interpretation of an event as stressful, but also our understanding of the role of life events depends on the models and links used by the researcher. Usually omitted in the causal chain of events are the broad politico-economic processes, which help structure the micro-situations within which individuals interact. The importance of these micro forces and social relationships are hidden by the focus on 'objective' events and the mitigating characteristics of individuals (Nzewi 1989).
For example, just as we can become narrowly focused when we study people only at a certain age, we can also miss important aspects by studying people from only one culture. Studying the differences in behaviour of people from different cultures can tell us a great deal about the origins and possible treatments of abnormal behaviours. Unfortunately, most research literature originates in Western cultures, producing an ethnocentric view of psychopathology that can limit our understanding of disorder in general and can also restrict the way we approach treatment. Cook's (1994) research findings have revealed cultural variability according to the extent that different cultures subscribe to biomedical, psychosocial and phenomenological beliefs about chronic illness.
Furnham (1997) also notes further that cultural attitudes towards illness particularly affect the availability of professional help. The issue of acceptability of professional help is particularly important, because if a cure is recommended to a patient who does not believe in the theories of the cause and/or cure of an illness, the patient suffering from such illness may not follow the guidelines for the cure or may ensure that the cure is ineffective. The theories of cause and cure of diseases must of necessity be meaningful to the patient in terms of the realities he/she understands.
Increasing awareness of the limited cultural scope of our research is creating a corresponding increase in cross-cultural research on psychopathology and psychotherapy.
Also, the characteristics of different cultures can also reflect on the symptom report. Symptoms or descriptions of them can be very dissimilar in different societies. For example, Nigerians who are depressed complain of heaviness or heat in the head, crawling sensations in the head or legs, burning sensations in the body, and a feeling that their belly is bloated with water (Ebigbo, and Ihezue 1982). By contrast, people in the United States report feeling worthless, being unable to start or finish anything, losing interest in usual activities, and thinking of suicide. Natives of China, on the other hand, do not report loss of pleasure, the helplessness or hopelessness, guilt, or suicidal thoughts seen in depressed North Americans (Kleinman, 1980). Again, many symptom reports of depression among Africans do not result in suicides. These few examples illustrate that applying a standard definition of depression across different cultures will result in vastly different outcomes.
On psychotherapy, what happens when people seek psychotherapeutic help? According to Sue & Zane (1987), seeking such help is related to one's ethnic background. Researchers in the United States of America have found that mental health services for minority groups are inadequate. As evidence of this problem, Stanley Sue (1992) cites statistics indicating that Blacks, Native Americans, Asian-Americans, and Hispanics tend to terminate psychotherapeutic treatment earlier and also average fewer sessions than whites. Between 42 and 55% of minority clients failed to return after a single session, compared to a 30% dropout rate for white clients. Among the reasons for these findings are a lack of bilingual therapists and therapists' stereotypes about ethnic clients. The single most important reason may be that therapists do not provide culturally responsive forms of therapy. They may also be unaware of values and customs within a culture that would help in understanding and treating certain behaviours.
To counter the high rate of early termination of treatment by minority clients, some psychologists have suggested that therapists develop greater cultural understanding and knowledge. In addition, therapists from diverse ethnic backgrounds and ethnic-specific therapeutic services are needed. There is also a need for more bilingual and bicultural personnel who could work more effectively with clients from different cultures and with those for whom English is a second language.
How does culture sensitivity affect psychotherapy? Sue, Fujino, Hu, Takeuchi, & Zane (1991) analysed the services, length of treatment, and outcomes of therapy for several ethnic groups in the Los Angeles mental health system. Ethnic match (in which the client and therapist were members of the same ethnic group) was related to length of treatment and was also associated with success of treatment among Mexican Americans. Also, the study showed a long-lasting and successful treatment, when clients for whom English was not their primary language have the same ethnic background and spoke the same language as the therapist. The researchers concluded "match is important because it is related to length of treatment".
Concluding comments
It is possible that views and observations concerning the African client in this paper will be increasingly incorporated into understanding disease classification and the implications it also has for psychotherapy practice during the coming years. Such a process would represent the current globalization in the mental health sector. It is from a perspective of social and cultural change, then, that we must consider the current utilization of mental health resources among Africans, particularly those living abroad. This process would mean an integration of some sorts.
However, many questions remain, concerning how such integration might occur. One area of concern is how these beliefs systems can be measured and whether such methods would be subject to adequate empirical testing and outcome research before they become widely used. On the other hand, depending on how these and related concerns are resolved, is it possible that empirically validated, spiritually oriented, integrative psychotherapeutic forms will emerge within a contemporary Western framework?
In the words of Nzewi (1989), "the major issue in the understanding of diagnostic categories and aetiological factors in other cultures is not merely discovering equivalence of concepts cross-culturally or matching patterns of symptoms". More important than these factors is the understanding of the vocabulary, belief system and the perceptions of the patients. The aetiology and symptom presentation of patients are often functions of culture. For example, though the clinical picture presented in delusional and hallucinatory states may be the same trans-culturally, it is obvious that cultural beliefs, environmental factors and the nature of interpersonal relationships all determine the contents of the delusions and hallucinations.
According to Sollod (1993), it is unfortunate that Western psychology has tended to de-spiritualize psychotherapeutic endeavor, thereby overlooking the spiritual dimensions of life and of experience. According to him, a wide range of spiritual healing traditions emphasizes the central importance of the connection of all life to spiritual or cosmic realities. In these views, healing is usually seen as restoring a condition of wholeness or harmony (Carlson & Shield, 1989). Contemporary psychology and many contemporary psychotherapeutic approaches express the perception of human beings as cut off and isolated, not only from nature and from other individuals, but also more significantly from activities of cosmic purpose. Copernican, Newtonian and Freudian conceptual revolutions have led to the notion of human beings as purposeless, determined organisms, acted upon by physical and biological laws. Even in humanistic approaches, meaning is usually seen as a subjective and arbitrary creation (Tart, 1987). According to him, contemporary psychotherapy has much to gain from a worldview that reconnects human beings with one another and with universal and spiritual purposes (Bergin, 1980).
Is the call for a merger of the rational approach with cultural dimension to be seen as a way forward in the effort to assist victims to overcome their emotional and mental disorders? To consider the roles of cultural experiences in dealing with human problems, especially in understanding the fears and aspirations, which often have become the causes of health problems (see Buhrmann (1984) and Collin and Sollod (1991), should therefore be the major concern of psychologists working with African clients. It is the task of psychologists to explore, for proper understanding and diagnosis, the effects of cultural influences on mental illness.
In conclusion, the current practice of Western psychotherapy in Africa must be revised. Psychotherapy without cultural justice can be better termed placebo-psychotherapy. It is without substance and is void of healing power (Idemudia 2002). Grossly, psychotherapy is measured in terms of total quality of human life. In the words of Awaritefe (1997) "a science which is oblivious of its cultural environment condemns itself to irrelevance.
© Erhabor Sunday Idemudia (Ibadan/Nigeria)
Contact: s.idemudia@iu-bremen.de
/ sundayidemudia@yahoo.com
REFERENCES
Awaritefe, A. (1997). The mind-body in an African context. Ife Psychologia: An International Journal, Vol. 5(1), pp. 140-149.
Ayorinde A. (1977). Heat in the head or body: A semantic confusion - Afric J Psychiat Vol. 1, pp. 59- 63.
Bergin, A. E. (1980). Psychotherapy and religious values. ]ournal of Consulting and Clinical Psychology, 48, 95-105.
Bourquignon, E (1989). Competition and complimentarity in the utilization of Health References - Africa in (Peltzer and Ebigbo, eds.) Clinical Psychology in Africa, Working group for African Psychology, University of Nigeria Enugu-Nigeria.
Buhrmann, M. V. (1984). Living in two worlds: Communication between a white healer and her black counterparts. Cape Town: Human & Rousseau.
Carlson, R., & Shield, B. (1989). Healers on healing. Los Angeles: Tarchef.
Collin, S., & Sollod, R. (1991). The relevance of traditional healing for psychotherapy: Content arid/or context. Paper presented to the 6th Annual Convention of the Society for the Exploration of Psychotherapy Integration, Philadelphia, PA.
Cook, P. (1994) Chronic illness beliefs and role of social networks among Chinese, Italian and Angloceltic Canadian. Journal of Cross-Cultural Psychology 25: 452-465.
Ebigbo, P.O. (1989). The Mind, the body and Society: An African Perspective. In K. Peltzer and P.O. Ebigbo (ed.). Clinical Psychology in Africa. Enugu, WGAP, 482-484.
Ebigbo, P.O. and Ihezue U.H. (1982). Uncertainty in the use of western diagnostic illness categories for labelling mental illnesses in Nigeria. Psychosomatic Africaine 3 XVIII(1), 59 - 74.
Ezeabasili, (1977). African Science, Myth or Reality? New York: Vantage Press.
Fridah-Muyale-Manenji (1998). The effects of globalisation on culture in the eyes of an African woman. Http://www.wcc-coe.org
Furnham (1997). Overcoming Neurosis. Lay attributions of cure for five specific disorders. Journal of Clinical Psychology, 53, 595-604.
Gordon, J. S. (1990). Holistic medicine and mental health practice: Toward a new synthesis. American Journal of Orthopsychiatry 60(3), 357-370.
Harkness, S and Keefer, C.H. (2000). Contributions of cross-cultural psychology to research and interpretations in education and health. Journal of Cross-Cultural Psychology, 31, 92-109.
Idemudia S.E. (1995). A Therapeutic Confrontation approach to treating refugees with progressive Psychopathology: Specific Problems and techniques. African Journal for the Psychological Study of Social Issues, Vol. .2, (1&2), 176-185.
Idemudia S.E., (2003). Tradotherapy and Psychotherapy in Africa: A Synthesis. In Sylvester Madu (Ed.) Contributions to Psychotherapy in Africa. UNIN Press. The University of the North for the World Council for Psychotherapy, African Chapter, South Africa, pp. 32-44.
Idemudia, S.E. (2002). Psychotherapy practices in Nigeria. In Alfred pritz (Ed.) Globalised Psychotherapy. Facultas Universitatsverlag-und Buchhandels AG, Vienna, pp. 575-592. Bergasse (For World Council for Psychotherapy (WCP)-Austria.
Innes, J. (1981). Social Psychological Approaches to the study of the induction and Alleviation of Stress: Influences upon Health and illness. In G. Stephenson and J. Davies (ed.) Progress in Applied Social Psychology. Chichester: John Wiley and Sons, pp. 155-190.
Kleinman, A (1980). Patents and Healers in the context of culture. Berkeley, University of California Press.
Lambo, T.A. (1963). Psychosomatic disorder in West Africa. WHO Technical Report Series 275.
Lambo, T.A. (1978). Psychotherapy in Africa. Human Nature, 1(3), 32-39.
Madu S.N., & Idemudia S.E. (1997). Traditional healer's approach to the treatment of apoplexy (Hemiplegia) -Paralytic stroke (A case study in Nigeria. In S.N., Madu, P.K., Baguma, and Alfred Pritz, (Ed); African Traditional Healing (Psychotherapeutic Investigation). Vienna: Austria Facultas Universitaetsverlag Berggasse 5, A-1090. Pp. 175-181.
Matsumoto, DC. (1996). Culture and Psychology - Boston , Brooks Kole.
Morakinyo O. (1985). Phobic States presenting as somatic complaints syndromes in Nigeria: Socio-cultural factors associated with diagnoses and psychotherapy. Acta Psychiatar Scand, 71, 356-365
Mume, J. (1974). Traditional Medicine in Nigeria. Agbaro: John Nature Cure Centre.
Nefale, M.C. and Van Dyke, G.A.J. (2003). Ubuntu Therapy - A Psychotherapeutic model for the African Client. (In Madu S Ed) Contributions to Psychotherapy in Africa. South Africa: The University of the North Press for the World Council for Psychotherapy.
Nzewi, N. Esther (1989). Cultural factors in the classification of Psychopathology in Nigeria. In K. Peltzer and P.O. Ebigbo (eds.). Clinical Psychology in Africa. Enugu, WGAP, pp. 208-216.
Okhomina, F.O.A and Ebie, J.C. (1973). Heat in the head as a Psychiatric symptom (In Adonakoh C.C. ed) Proceedings of the 4th Pan Africa Psychiatric Congress workshop on Neurosis in Africa - Accra: New Times corporation.
Pearce, T.O. (1989). Social organization and Psychosocial Health (Peter, K and Ebigbo, P ed) Clinical Psychology in Africa, pp. 47 - 55).
Prince, R (1975)..Some Yoruba views of the causes and modes of treatment of anti-social behaviour. Afric J Psychiat, 2 (133- 7)
Sollod R.N. (1993). The Comprehensive Handbook of Psychotherapy integration (George Stricker and Jerold R. Gold eds) Plenum Press, New York.
Sue S. (1992) Cited in Sue, D., Sue, D., & Sue, S. (1997). Understanding Abnormal Behaviour. New York: Houghton Mifflin Company.
Sue, Fujino, Hu, Takeuchi, & Zane, (1991). Response of African American and Caucasian Women to Cognitive Behavioural Therapy for PTSD. Behaviour Therapy, Vol. 30, 581-595.
Sue, S. & Zane, N. (1987). The role of culture and cultural techniques in
psychotherapy: A critique and reformulation. American Psychologist, 42, 37-45.
Tart, C. (1987). Waking up: Overcoming the obstacles to human potential. Boston: Shambala.
Taussing, M (1980) - Reification and the consciousness of the Patent. Social Science and Med Vol. 14B (pp. 3-13)
Tsa-Tsala (1997). Beliefs and Disease in Cameroon. In S.N. Madu, P.K. Baguma and Pritz, A. (eds.) Psychotherapy in Africa: First investigation. Vienna. World Council for Psychotherapy, pp. 44.
Van Der Walt, B.J. (1997). Afrocentric or Eurocentric? Our task in a multicultural South Africa. Potchefstroom: pu for CHE
2.7. Culture, Psychosocial Disorders and Mental Health: an African Perspective
Sektionsgruppen | Section Groups | Groupes de sections
![]() Inhalt | Table of Contents | Contenu 15 Nr.
Inhalt | Table of Contents | Contenu 15 Nr.